 The rate of suicide has increased dramatically across most segments of our population in recent years. According to the National Institute of Mental Health, there were more than twice as many suicides in the USA in 2017 as there were homicides. The Military Veteran Project is actively engaged in improving brain health and mental health by providing research and treatment not available or accessible by the VA or DOD to veterans around the world. We are committed to spreading awareness of this distressing issue. Suicides affect many segments of the population, and various factors contribute to this epidemic. Chronic illnesses, both mental and physical, increase suicidal ideation in those who have suffered for years, Military veterans are more likely than the civilian population to develop mental health problems, such as post-traumatic stress disorder, depression, and traumatic brain injury. Veterans are also at high risk for developing associated substance-use disorders – all factors associated with suicide. Everyone can play a role in suicide prevention. Major mental illnesses rarely originate “out of the blue,” and oftentimes family, friends, teachers and/or the individuals themselves can learn to recognize small changes before the point of no return. Symptoms listed here, including withdrawal, apathy, social isolation, unusual behaviors, and mood changes, are early warning signs that can be brought to a mental health professional’s attention. Suicides are preventable, and the stigma surrounding mental health problems can and should be addressed in our society. Military traumatic brain injury and its consequences are at a crisis level. There are medical facilities, non-profit organizations and people across the county and around the world that are prepared to unite to fight for the freedoms our veterans deserve when they return home from war, even a simple freedom of proper diagnosis. Since 2012, the Military Veteran Project's small grassroots movement has made huge momentum from Washington DC to Los Angeles to Texas up to Minnesota and even over seas in Europe and the middle east and we know we must continue our efforts. In September each year, our fellow medical facilities and supporters across the country will place 22 white crosses to represent the number of estimated veteran suicides that happen each day. We do not want to forget the sacrifice made by our veterans or their families that left behind. Please join us by simply creating your own "memorial" and alert your local media of the nationwide event. If you are a veteran looking for answers to your questions and need help, please contact us. Click below to join us to help create changeIntroduction
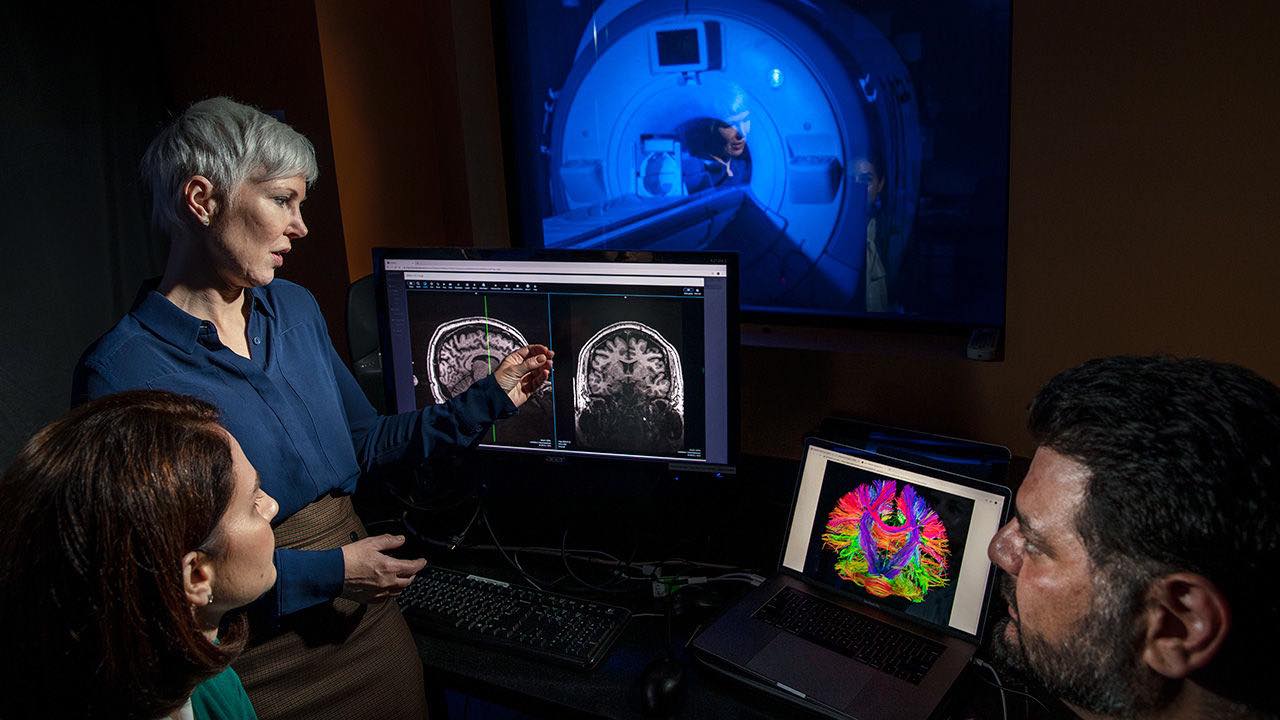
Suicide is a significant public health concern, especially for U.S. military personnel and veterans and has been identified as one of the leading causes of death in the U.S. military (Armed Forces Health Surveillance Center, 2014). Moreover, the suicide rate among U.S. veterans reportedly increased between 2001 and 2014 and risk for suicide in veterans was 21% higher than in the US civilian adults, after considering the differences in age and gender (Office of Suicide Prevention, 2016). Rates of veterans who die by suicide have increased public attention to suicide and underscored the need for research to identify risk factors and to increase suicide prevention efforts in veterans and military personnel (Ramchand et al., 2011; Department of Veterans Affairs, 2013). To date, various interventions ranging from individual to community level approaches are being scrutinized and employed for the prevention and treatment of suicide. However, a limited number of approaches in screening, prevention and treatment have been supported by empirical evidence in part due to the complexity in the psychopathology of suicide in the context of various psychiatric disorders including major depressive disorder (MDD), bipolar disorder, anxiety disorders, and substance-related disorders (Klonsky et al., 2016). A stress-diathesis model of suicide behavior proposed by Mann and his colleagues included stressors in the lifetime and vulnerability of individuals as its components (Mann et al., 1999). In essence, when individuals with suicidal diathesis including genetic, epigenetic, and other neurobiological vulnerabilities encountered distress caused by psychiatric disorders and adverse psychosocial events, he or she would be more likely to demonstrate suicide behaviors. Suicide behaviors are defined as self-directed injurious acts with at least some intent to end one's own life (Mann, 2003). Notably, a majority of psychiatric patients do not exhibit suicide behaviors, while >90% of individuals who die by suicide may be diagnosed as having any psychiatric disorders (Bertolote and Fleischmann, 2002; Nordentoft et al., 2011). This observation was consistent with a crucial role of diathesis in the model of suicide behaviors. Moreover, it has been acknowledged that most individuals with suicidal ideation do not attempt suicide (Kessler et al., 1999; ten Have et al., 2009). The critical need for differentiating suicide attempters from suicide ideators has been identified in research on suicide (Klonsky and May, 2014) and investigating the neurobiological diathesis for suicide behavior would address this need. In fact, several structural and functional brain imaging studies on subjects with suicide ideation or history of attempt have been conducted to identify neurobiological differences along the suicide diathesis (Cox Lippard et al., 2014; van Heeringen et al., 2011).
0 Comments
For those people who want to apologize to Iran for the killing of Qassem Soleimani, I present you with Army Captain Brian S. Freeman. Brian was a loving husband, father, Olympic caliber athlete and Army Civil Affairs team leader who actually cared about people regardless of who they were, where they came from, what God they worshipped, or their politics. 13 years ago this month, Cpt. Brian Freeman and his team of Civil Affairs soldiers were in Karbala, Iraq at a meeting to help improve the lives of the people of that province. During that meeting, a team under the command of Gen. Qassem Soleimani, stormed in, killing a number of American's, and capturing Brian and several members of his team. The captured CA team members were handcuffed, driven away from the meeting and later executed. Once found, in spite of our best efforts, several medics, unsuccessfully attempted to save Brian. Captain Freeman is but one of the lives lost due to the evil of Qassem Soleimani. Qassem Soleimani was an evil person whose end, regardless of the politics surrounding it is a good thing. Rest In Peace, Brian. This was a view submission.
Thank you Jennifer who created this post for your perspective. The U.S. State Department is urging all U.S. citizens to leave Iraq after the New Year's Eve attack on the embassy in Baghdad by Hashed al-Shaabi, a pro-Iranian paramilitary group, that caused extensive damage to the property.
"On December 31, 2019, the Embassy suspended public consular services, until further notice, as a result of damage done by Iranian-backed terrorist attacks on the Embassy compound," the State Department said in an update to its Iraq travel advisory on Wednesday. Photos show a burned and charred reception area, smashed windows and vandalized rooms left behind by supporters and members of the Iranian-trained Hashed al-Shaabi military network, also known as the Popular Mobilization Forces. No deaths or serious injuries have been reported, and the embassy was not evacuated. In response, the Pentagon deployed 750 paratroopers from the 82nd Airborne,based at Fort Bragg, North Carolina, to the region. Your actions can forever change the lives of someone in need'
MISSION: The basic mission of the Marine Toys for Tots Program is to collect new unwrapped toys and distribute those toys to less fortunate children at Christmas.
GOAL: The primary goal of Marine Toys for Tots is, through the gift of a new toy, help bring the joy of Christmas and send a message of hope to America's less fortunate children. OVERVIEW: In order to better execute the Program, in 1991 the Marine Toys for Tots Foundation was created at the behest of the Marine Corps. FOUNDATION OVERVIEW: The Marine Toys for Tots Foundation, is an IRS recognized 501(c)(3) not-for-profit public charity which was created at the behest of the U. S. Marine Corps in 1991. FOUNDATION GOVERNANCE: The Marine Toys for Tots Foundation is governed by a board of directors, all of whom are veteran Marines and successful business leaders from throughout the nation. The Foundation’s professional staff is headquartered in the Cooper Center, which is located just outside the Main Gate of Marine Corps Base, Quantico, about 35 miles south of Washington, DC. FOUNDATION MISSION: The mission of the Marine Toys for Tots Foundation is to assist the U. S. Marine Corps in providing a tangible sign of hope to economically disadvantaged children at Christmas. This assistance includes providing day-to-day leadership and oversight of the Program, raising funds to provide toys to supplement the collections of local Toys for Tots Campaigns, to provide promotional and support material and defray the costs of conducting annual Toys for Tots Campaigns. Other Foundation support includes providing administrative, advisory, financial, logistic and promotional support to local Toys for Tots Coordinators; managing funds raised and monies donated based on the use of Toys for Tots name or logo; providing other support the Marine Corps, as a federal agency, cannot provide; and conducting public education and information programs about Toys for Tots that call the general public to action in support of this patriotic community action program. FOUNDATION OBJECTIVES: The objectives of the Foundation are to help less fortunate children throughout the United States experience the joy of Christmas; to play an active role in the development of one of our nation’s most valuable resources – our children; to unite all members of local communities in a common cause for three months each year during the annual toy collection and distribution campaign; and to contribute to improving communities in the future. FOUNDATION ACTIVITIES: The Foundation engages in two categories of activities: Program Services and Support Services. Program Services Collection and Toy Distribution: This is the process of obtaining and delivering toys to local Toys for Tots Coordinators and providing the support and assistance those Coordinators need to conduct effective toy collection and distribution campaigns in their communities. Toy collection includes a combination of locally donated toys, those purchased by the Foundation, and those donated by corporations. Support of Local Coordinators: This involves arranging the creation, publication, manufacture and delivery of an array of promotion and support materials to local Coordinators. It includes managing all financial matters for local Coordinators as well as updating and publishing a manual for the conduct of local programs. Concisely stated, this activity encompasses providing a wide range of support to nearly 800 local Toys for Tots Coordinators and their support groups. Today, there are nearly 40,000 Marines, Marine Corps League members, veteran Marines and volunteers involved in annual campaigns. Education: The Foundation conducts an annual public information and education campaign. This activity is designed to give the general public a clear understanding of the benefits that accrue to individuals, communities and the nation from Toys for Tots. It increases visibility and name recognition, and calls the general public support in Toys for Tots. The campaign includes distributing a series of news releases, distributing TV and radio public service announcements, publishing newsletters arranging media events and appearances, arranging for national corporations to incorporate information about Toys for Tots into their paid advertisements, conducting special events, maintaining a website and distributing educational material about Toys for Tots to the general public. Support Services Management and General Activities: This involves accomplishing the spectrum of business management activities necessary to make an organization efficient and effective and to ensure the program and the Foundation operate in compliance with IRS regulations, federal and state laws and charitable standards. Fundraising: The Foundation pursues a range of fundraising projects each year. Projects include national corporate sponsors, a direct mail campaign, the Combined Federal Campaign, special events such as golf tournaments; and special projects such as “in memory of/in honor of” donations and internet donations. PERFORMANCE and ACCOMPLISHMENTS: Since 2001 ranked as one of the top rated charities by “Philanthropy 400” Unmodified opinions on Audited Financial Statements (1994-2017) Average Program to Support Service expense ratio: (2000-2017) 97:3 Continues to meet all 20 standards established by the Better Business Bureau WiseGiving Alliance Earned Charity Navigators (www.charitynavigator.org) Four Star Rating Patient and Veterans advocates, industry leaders, and non-profits call on Congress to support “100 days faster” clinical trial startup at the U.S. Department of Veterans Affairs May 16, 2019 - PRESS RELEASE Contact: Roger Murry, Executive Director, Coalition to Heal Invisible Wounds WASHINGTON, D.C. – A coalition of organizations that support research at the U.S. Department of Veterans Affairs (VA) this week called on Congress to support reforms at the VA to become “100 days faster” in clinical trial startup to ensure enhanced and timely access for our nations Veterans. “Clinical trial startup at VA sites averages more than 100 days longer than at non-VA sites,” according to the letter sent to Congress. “For Veterans suffering from post-traumatic stress disorder, traumatic brain injury, hearing loss, alcohol and other substance disorders, cancer, and other conditions for which a clinical trial may be the next or only treatment option, these delays can restrict their access to these opportunities.” The Coalition to Heal Invisible Wounds and National Association of Veterans’ Research and Education Foundations (NAVREF) organized the letter. Joining the letter were organizations that serve Veterans, including the Navy SEAL Foundation, Military Veteran Project, and NAMI Montana. Patient support groups signing included the Prostate Cancer Foundation, Veterans Against Alzheimer’s, and the LUNGevity Foundation, the nation's leading lung cancer-focused nonprofit. Representatives of the research community supporting the letter included PPD, Cohen Veterans Bioscience, Advantagene, and the Association of Clinical Research Organizations. The letter continued: “As a first step towards ‘100 days faster,’ which we suggest the VA adopt as a reform mantra, we ask that the VA take all steps necessary to permit the use of commercial IRB [institutional review boards] accredited by the Association for the Accreditation of Human Research Protection Programs (AAHRPP). This policy revision would allow for a more predictable and timely IRB process.” The letter seeks to engage congressional support for an ongoing effort co-led by the VA Office of Research and Development and NAVREF to improve access of Veterans to clinical trials. By setting an objective, measurable goal of 100 days faster, the VA can drive reforms throughout the clinical trial process, whether within the purview of ORD or not. Targeted reforms, beginning with allowing trial sponsors to use commercial institutional review boards, can bring VA’s practices in line with those of the leading clinical research institutions. “Clinicians need better tools to treat and diagnose TBI and PTSD” said Roger Murry, Executive Director, Coalition to Heal Invisible Wounds, an advocacy coalition based in Washington, DC. “Smarter clinical trial startup procedures will broaden and speed up the development of new tools. With targeted support from Congress, and the concrete goal of 100 days faster, we believe VA can close the gap and change how the private sector views the VA as a potential clinical trials partner.” “NAVREF appreciates ORD’s strong support of the ACT for Veterans initiative to enhance access to clinical trials for Veterans at VA medical centers, said Rick Starrs, the Chief Executive Officer for NAVREF. We want to see the entire Veterans Health Administration get behind the initiative to achieve the goal of 100 days faster for clinical trial start-up. Veterans deserve the opportunity to participate in these studies.” More info can be found at healinvisiblewounds.org ***
Joshua Russell Akers, beloved of his wife Victoria Mizell Akers, committed suicide on March 8, 2019. A 2006 graduate of Plano Senior High and Wild Cat Football team, Joshua proudly served our country as a Sergeant in the United States Marine Corps for 5 years.
Josh was pursuing his degree in Petroleum Engineering at UNT where he was a member of The Association of Energy Engineers, Kappa Alpha, and The American Society of Mechanical Engineers. Outside of school, Joshua enjoyed woodworking, gaming, his puppies, and spending time with friends and family. Joshua was the light of our lives. His laughter was contagious and he was a good and loving husband, son, brother, cousin, and friend. He was a leader, and powerful influence on all who knew him. He inflicted his dad jokes and humor on all who would listen, and was always ready with random trivia, a word of advice or just a listening ear. Joshua is survived by his loving wife, Victoria Mizell Akers, his Mother Sara Egelston Akers and Father Jeran Akers and wife Victoria Harres, brother, Ty Akers, and sister, Jan Michael Wells. Josh is also survived by his aunts and uncles Rebecca Egelston Caso and Chris Caso and John and Gena Egelston and grandmother Marcia Stathos Egelston. Josh will be missed by his cousins Christopher and Catherine Caso, and James Russell and Andrew Egelston. The services were on Saturday, March 16 at 2 p.m. at Christ United Methodist Church, 3101 Coit Road, Plano, Texas. FFor Immediate Release
Military Veteran Project Partners with Hestons Gladiator upcoming event OrganizedChaosXVI for Military Suicide Awareness Military Veteran Project and Hestons Gladiator Academy are partnering to combat military suicide by honoring men and women who have lost their battle to suicide on American soil this Saturday, May 18, 2019 7pm at Historic Harley Davidson. TOPEKA, Kansas – Heston's Gladiator Academy to combat military suicide by honoring men and women who have lost their battle to suicide on American soil this Saturday, May 18, 2019 7:00pm at Historic Harley Davidson. Organized Chaos XVI will be dedicated to military men and women who have lost their battles on American soil to suicide by displaying boots with photos and biographies for community outreach. MVP Ambassador Colton Hill will be leading the charge to combat Military Suicide by fighting in honor of a veteran who succumbed to suicide. The Military Veteran Project is a 501c3 charity dedicated to military suicide prevention by providing research and treatments not provided by the VA or Department of Defense. Gladiator Fighting Association https://www.cagetix.com Military Veteran Project needs your help to battle military suicide prevention. We can’t do it alone – and your donations make a huge difference for the veterans who return home after service.
Starting at 5am on November 27th, Facebook will MATCH ALL DONATIONS from $100 – $20,000 per person until we reach $250,000 or Facebook runs out of money. That means if you donate as little as $7 which is the cost of one treatment, Facebook will match it! If you can not donate please help us get out the word by liking, commenting and sharing this event and our mission! #EndMilitarySuicide Visit the MVP Facebook page November 27th and click on the “Donate” button or create a fundraiser on your own and join our mission https://www.facebook.com/fundraisers?sem_campaign_id=1522769271.57275788974.312079087912.EAIaIQobChMIjLbW-M_l3gIVUL7ACh2JEwG_EAAYASAAEgLjDvD_BwE&sem_adgroupid=c.kwd-312250270023&sem_keyword=%2Bfacebook%20%2Bfundraising
Whether you make a donation to a cause in place of party favors or ask your guests to invest in a charity instead of a crock pot, a little selflessness can go a long way for many non-profits—and experts say the practice is becoming more and more popular for engaged couples. Why? Lizzy Ellingson, co-founder and chief creative officer of Blueprint Registry, explained to Brides where this spike in charitable registries came from. "Millennials are cohabiting before marriage and getting married later in life," she says. The material needs of a 21-year-old just starting out are different from a couple of 30-somethings who have already been living together. Additionally, "Crowdfunding has exploded in popularity over the past 10 years growing at 26 percent a year. Based on proprietary research, Blueprint Registry estimates that cash gifting and personal crowdfunding will exceed $33.5 billion by 2021," Ellingson says. She expects this to heavily impact wedding registry trends, as well—her company has already seen this shift start to happen. "At Blueprint Registry," she continues, "70 percent of couples register for at least one cash gift like a honeymoon plane ticket or contributions to help with remodeling a kitchen. We still see couples register for both physical and cash gifts, we just see more couples register for cash who may not have registered for any cash gifts five years ago." The increase in popularity for cash registries demonstrates that even for "the couple who has everything," there is a way for guests to celebrate the union with a gift. It's also a good option to help ease the financial burden for guests who might already find it challenging to accommodate the cost of attending the wedding (think destination weddings and multi-day celebrations). Just like with any crowdfunding, there's security in numbers—each individual doesn't feel obligated to fork over the same amount they might for a more traditional, high-quality registry item, and that's fine. Blueprint found that while the average fundraising goal for charitable registries is just under $900, and the average amount raised is a little less than half of that. An idea for couples who want to keep their guests motivated to give more: if your budget allows, agree to match their donations up to a certain amount. You'll do good for the community and the world, plus you'll get an even bigger tax write-off. You can also think small if you'd like. A charitable registry—or swapping out wedding favors to donate money in your guests' names—can have a more local impact, too. Blueprint Registry offers an option to create a cash registry for local charities as well, which has become the most common choice among couples on the site. Choosing which organization will be gifted with your support can be overwhelming—but with so many worthy causes, you can't go wrong choosing something personal to you and your fiancé. A couple who has lost a family member to suicide might donate to research efforts around prevention like the Military Veteran Project. This is just another way to personalize the wedding celebration while giving back. Whatever you choose, know that you're making a difference by paying all that wedding generosity forward. For Immediate Release:
Topeka, KS (December 6, 2017) -- Military Veteran Project, a national military charity with a mission of military suicide prevention through alternative treatments and research created the Salute Our Heroes Festival & Topeka Veterans Parade as a program for community outreach. After the fifth annual event this year the MVP Board of Directors voted unanimously to transfer the program to another organization due to the alarming rate of suicides increasing and the need to focus forefront on the mission of military suicide prevention. “The volunteers of the Military Veteran Project have created a much needed program for our Topeka community, our local veterans deserve to be recognized and honored. However, our mission as the Military Veteran Project is military suicide prevention and with the numbers of suicides increasing each day, our focus needs to be solely on ensuring the needs of our veterans are being met by continuing our work with the Department of Defense, Veterans Administration, Medical Researchers and Corporations providing alternative treatments not currently available. In 2012, when I decided to create the first ever Topeka Veterans Parade, my hopes for a couple hundred of people to help honor veterans turned out to be thousands. We have a committed committee of volunteers who have surpassed all expectations I have had and I want to personally thank Michael Majewski, Penny Jamvold, Dusty Nichols, Richelle Blume-Shannonhouse, Ron Brown, Amanda Walton & Glen King for their commitment to veterans and our Topeka Community.” To assist with the momentous task of selecting and transitioning the Salute Our Heroes Festival & Topeka Veterans Parade to a 501c3 charity locally, a sub committee of Topeka Community leaders have been selected to process interest requests and finalize the selection process. Military Veteran Project volunteers, ambassadors and committee members will assist with handover process and transition to the new organization to assist carry on the mission to honor our military heroes. Any and all interested parties may submit letters of interest to [email protected] or by mail Military Veteran Project 3615 SW 29th Street Suite 201 Topeka, KS 66614 Very Respectfully, Melissa D. Jarboe Founder Military Veteran Project |
Sign up for our mailing list by clicking here
Archives
March 2020
|
||||||||||
|
Get to know us
|
Resources
|
Get Involved
|
|
|
|
|
The Military Veteran Project is a non-profit 501 (c)3 organization, IRS identification number 46-0877378. Donations made to the Military Veteran Project are tax deductible in the U.S. ·











 RSS Feed
RSS Feed